What stubborn problems in microcirculation can Oxpentifylline overcome?
Oxpentifylline is a core pharmaceutical raw material belonging to the methylxanthine class. Its unique heterocyclic skeleton and alkyl side chain combination create its distinctive physicochemical properties and bioactivity. Under normal conditions, it is a clean, white crystalline powder with excellent water solubility and compatibility with organic solvents, meeting the quality control standards for pharmaceutical-grade active pharmaceutical ingredients. Unlike ordinary xanthine derivatives, this raw material possesses a comprehensive effect of simultaneously optimizing blood rheology, repairing vascular endothelial homeostasis, alleviating low-grade inflammation, and regulating systemic metabolic circulation. It has extremely high application value in clinical scenarios such as peripheral vascular dysfunction, weakened cardiovascular and cerebrovascular circulation, and metabolic-related microcirculatory imbalances.
The skeletal code of methylxanthine
Oxpentifylline is chemically 3,7-dimethyl-1-(5-oxohexyl)-3,7-dihydro-1H-purine-2,6-dione, a synthetic derivative of the methylxanthine class of compounds. Its molecular skeleton is centered on xanthine, a bicyclic structure formed by the fusion of a pyrimidine ring and an imidazole ring, widely found in nature in coffee, tea, and cocoa beans. Oxpentifylline differs from caffeine and theophylline in its side chain modification—a 5-oxohexyl side chain is attached to the nitrogen atom at position 1 of the xanthine ring. This structural modification is the key molecular switch determining its pharmacological identity. This side chain not only alters the molecule's lipophilicity, allowing it to cross cell membranes more effectively, but also endows it with selectivity in interacting with the phosphodiesterase family, thereby transforming its original central excitatory effect into a peripheral vascular protective function.
In terms of molecular configuration, the xanthine core has a methyl group at positions 3 and 7, and these two methyl groups form a specific three-dimensional arrangement that influences the way the molecule binds to the target protein. The precise molecular formula of Oxpentifylline is C₁₃H₁₈N₄O₃, with a molecular weight of 278.31 g/mol and a calculated LogP value of approximately 0.86, indicating moderate lipophilicity—a characteristic that allows it to be soluble in aqueous media and penetrate biological membrane systems. Physically, high-purity Oxpentifylline is a white to off-white crystalline powder with a melting point between 102°C and 105°C, exhibiting good chemical stability under dry conditions at room temperature.
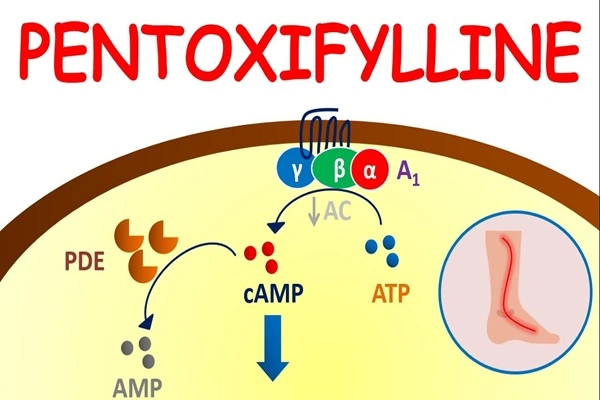
Structurally, Oxpentifylline has several equivalent chemical names, all of which are chemically identical. Its Chinese name, "hexanone-theobromine," originates from the "hexanone" structure in its side chain and the "theobromine" skeleton in its parent core. From a medicinal chemistry perspective, Oxpentifylline belongs to the first-generation phosphodiesterase inhibitors, targeting phosphodiesterase, the enzyme that degrades intracellular cAMP. By occupying the catalytic active site of this enzyme, Oxpentifylline slows down the hydrolysis rate of cAMP, maintaining or even increasing intracellular cAMP levels. cAMP, as a classic "second messenger," plays a central role in regulating vascular tone, platelet aggregation, and inflammatory responses; this is the molecular source of Oxpentifylline's pleiotropic pharmacological effects.
Regarding quality control, the production of Oxpentifylline active pharmaceutical ingredient (API) must strictly adhere to pharmacopoeia standards. Key quality control indicators include content determination, related substances, loss on drying, and heavy metal limits. Because Oxpentifylline is light-sensitive, the API should be stored in a light-protected, airtight container in a cool, dry place. Its sustained-release tablets typically utilize special matrix materials to control the drug release rate, maintaining stable blood concentrations over 12 hours; this is the pharmaceutical basis for its three-times-daily dosing regimen.
Dual pathways for blood flow optimization
The pharmacological action of Oxpentifylline can be understood as a "two-track" logic—it improves both the "flow properties" of blood and reduces its "coagulation tendency." At the level of blood rheology, oxpentifylline increases cAMP levels within erythrocytes, activating cAMP-dependent protein kinase A, which in turn phosphorylates erythrocyte membrane skeletal proteins. This series of phosphorylation events alters the membrane elasticity of erythrocytes, transforming them from a rigid "disc-like" shape to a more deformable form, allowing them to pass smoothly through capillaries smaller than their own diameter. Simultaneously, oxpentifylline inhibits platelet aggregation—by blocking downstream signaling from adenosine A2 receptors on the platelet membrane, reducing the release of calcium ions from platelets, thereby decreasing platelet adhesion and aggregation.
Regarding leukocyte-endothelial cell interactions, oxpentifylline exhibits a unique "anti-adhesion" effect. Under inflammatory or ischemic conditions, overactivated leukocytes adhere to the vascular endothelium, releasing proteolytic enzymes and free radicals, causing microvascular blockage and tissue damage. Oxpentifylline reduces the opportunity for leukocytes to "anchor" to the endothelium by inhibiting the expression of adhesion molecules on the surface of endothelial cells. In animal models of limb ischemia-reperfusion injury, oxpentifylline pretreatment significantly reduced neutrophil infiltration into ischemic areas and decreased the release of inflammatory mediators such as tumor necrosis factor-α, thereby alleviating tissue edema and necrosis after reperfusion.
At the hemodynamic level, oxpentifylline also has a certain vasodilatory effect. By increasing cAMP levels in vascular smooth muscle cells, it activates the phosphorylation regulation mechanism of myosin light chain kinase, causing smooth muscle to transition from a contracted to a relaxed state. This vasodilatory effect is particularly significant in skeletal muscle microcirculation, increasing blood perfusion in ischemic muscles and improving the oxygen supply-demand balance during exercise. However, unlike traditional vasodilators, oxpentifylline's vasodilatory effect is "mild and long-lasting," without causing significant hypotension or reflex tachycardia, which is its safety advantage as a treatment for peripheral arterial disease.
Oxpentifylline also affects the coagulation cascade by regulating the expression of tissue factor. Tissue factor is an initiator of the extrinsic coagulation pathway and is induced in the expression of monocytes and endothelial cells upon inflammatory stimulation. Oxpentifylline can significantly inhibit the expression of tissue factor induced by lipopolysaccharide or tumor necrosis factor-α, thereby reducing the initiation of thrombus formation. In a primate model of septic shock, intravenous injection of Oxpentifylline can block endotoxin-induced coagulation activation and reduce the risk of disseminated intravascular coagulation. This mechanism provides a pharmacological basis for its application in severe infections and thrombotic diseases.
Notably, the hemorheological effects of Oxpentifylline have a clear "therapeutic window." Animal experiments show that Oxpentifylline has minimal effect on the deformability of normal erythrocytes, only exerting a significant improving effect when erythrocytes are in a pathological "rigid" state. This "pathology-dependent" characteristic minimizes side effects under physiological conditions, consistent with the concept of "selective treatment." In addition, the metabolites of oxpentifylline also participate in maintaining the overall efficacy—its two main oxidative metabolites, M4 and M5, have a long half-life in vivo and have a stronger protective effect against tumor necrosis factor-α-mediated cytotoxicity.
Internal function regulation and physiology
Oxpentifylline's regulation of the body is not a simple action targeting a single point, but rather a multi-dimensional, simultaneous effort addressing blood rheology, vascular endothelial state, inflammatory mediator balance, and platelet physiological behavior. This multi-layered, interconnected approach constructs a complete microcirculation regulatory system, gently and persistently clearing blockages in microvascular circulation and repairing damaged circulatory homeostasis. Firstly, at the level of blood rheology, this ingredient gently alters the deformability and aggregation state of red blood cells, reducing overall blood viscosity. This allows red blood cells to pass smoothly through delicate capillaries, preventing blood stasis caused by cell aggregation and adhesion. When blood viscosity is high, red blood cells tend to clump together, slowing blood flow in microvessels, which can lead to microcirculatory ischemia and hypoxia over time. Oxpentifylline can reshape the surface mechanical properties of red blood cells, enhancing their deformability and passage ability, thus maintaining unobstructed blood perfusion in the peripheral microvessels throughout the body.
At the level of vascular endothelial maintenance, this ingredient can maintain the integrity of vascular endothelial cells and their normal physiological secretory function, reduce the continuous stimulation of the endothelium by adverse external factors, and slow down the process of microvascular hardening and elasticity loss. The vascular endothelium is a key barrier for maintaining vascular homeostasis. Factors such as metabolic disorders, high lipid stimulation, and long-term ischemia can gradually damage the integrity of the endothelium, leading to abnormal vascular permeability and decreased elasticity, thereby exacerbating microcirculatory imbalance. Oxpentifylline can alleviate the low-level stress state of endothelial cells, maintain the normal release of endothelial-related active substances, prevent abnormal vasoconstriction and excessive lipid deposition, and maintain the structural integrity and stable dilation and contraction rhythm of microvessels in the long term, thus slowing down the progression of microcirculatory lesions from the root cause.
The smooth regulation of inflammatory mediators is another core intrinsic characteristic of Oxpentifylline. It can moderately downregulate the expression level of low-level inflammatory mediators in the body, avoiding long-term damage to the microcirculatory system caused by long-term microinflammatory infiltration. In the progression of systemic microvascular disease, low-grade chronic inflammation is a constant companion, continuously attacking the vessel walls and surrounding soft tissues, exacerbating problems such as vascular stenosis, blood flow obstruction, and tissue malnutrition. This ingredient can gently counteract the overexpression of inflammatory mediators, weakening the invasive interference of microinflammation on blood vessels and peripheral tissues, creating a low-inflammatory homeostatic environment, and providing stable physiological conditions for microcirculation repair and tissue function recovery. Unlike the drastic intervention of potent anti-inflammatory components, its overall effect is gentle and suitable for long-term chronic disease management.
The benign regulation of platelet aggregation behavior is equally indispensable. Oxpentifylline can moderately inhibit the tendency of excessive platelet aggregation, reduce the probability of abnormal microthrombus formation in microvessels, and prevent microcirculatory pathways from being blocked by microthrombi. Excessive platelet activation and aggregation can easily form microemboli in delicate capillaries, blocking local blood flow and gradually inducing local ischemia, numbness, and ulceration. This ingredient gently balances platelet physiological activity, avoiding excessive inhibition of coagulation function and the risk of bleeding, while effectively reducing the potential for microcirculatory blockage caused by abnormal aggregation, achieving a balance between protection and safety.
Multi-dimensional regulatory logics intertwine and synergistically work together: blood rheology optimization unblocks basic blood flow pathways, vascular endothelial maintenance safeguards vascular structural homeostasis, micro-inflammatory regulation reduces persistent pathological invasion, and platelet activity balancing avoids microthrombus blockage. The entire mechanism of action is gentle and long-lasting without severe pharmacological impact, making it suitable for long-term applications such as long-term management of metabolic complications in middle-aged and elderly individuals, gradual intervention in chronic wound repair, and other long-term applications. It is precisely this multi-target gentle regulatory mechanism that distinguishes Oxpentifylline from ordinary vasodilators. It does not rely on simple vasodilation for short-term effects but rather repairs microcirculatory homeostasis from the physiological source, possessing the dual value of long-term maintenance and long-term prognosis improvement.
New Anti-inflammatory Domains and Delivery Innovation
In the field of ischemia-reperfusion injury, the organ-protective effects of Oxpentifylline have been better understood. When blood flow is restored to a limb, heart, or brain after ischemia, reperfusion itself triggers inflammatory responses and oxidative stress, causing "secondary injury." Oxpentifylline blocks this process through multiple mechanisms: it inhibits the inflammatory cascade induced by platelet-activating factor and endotoxin, reduces the recruitment of neutrophils to damaged tissues, and enhances the antioxidant capacity within tissues. In animal models of acute limb ischemia, Oxpentifylline pretreatment significantly reduced amputation and mortality rates, and the protective effect was further enhanced when used in combination with antioxidants such as vitamin C. These findings provide a theoretical basis for the perioperative application of Oxpentifylline in organ transplantation, cardiac surgery, and vascular interventional therapy.
Regarding drug delivery systems, the bioavailability of oral Oxpentifylline formulations has been a bottleneck in clinical application. Due to its limited water solubility and significant first-pass metabolism, the absolute bioavailability of conventional immediate-release tablets is only about 20% to 30%. To overcome this limitation, researchers have developed various novel delivery systems, including osmotic pump controlled-release tablets, gastric floating sustained-release systems, and nanoliposome carriers. A pH-responsive core-shell hydrogel microcapsule prepared using microfluidic technology, reported in 2026, can protect Oxpentifylline from gastric acid degradation and precisely release it in the alkaline environment of the colon. This "smart delivery" strategy not only increases drug concentration at the target site but also reduces systemic side effects by decreasing systemic exposure.
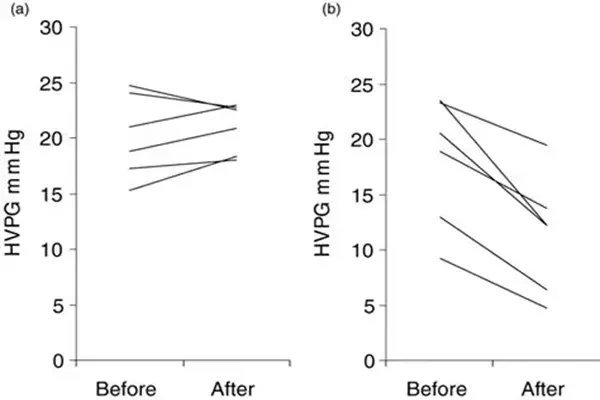
The application of Oxpentifylline in fibrotic diseases is another promising research direction. A common feature of pulmonary fibrosis, cirrhosis, and systemic sclerosis is the abnormal activation of fibroblasts and excessive deposition of the extracellular matrix. Oxpentifylline reduces collagen synthesis by inhibiting the transforming growth factor-β signaling pathway while increasing the activity of matrix metalloproteinases, promoting the degradation of deposited collagen. In the aforementioned diabetic nephropathy studies, the inhibitory effect of Oxpentifylline on glomerular sclerosis and interstitial fibrosis has been preliminarily confirmed. Future clinical trials specifically targeting patients with idiopathic pulmonary fibrosis and cirrhosis are needed to verify its anti-fibrotic efficacy.
Conclusion
Oxpentifylline, with its unique methylxanthine heterocyclic skeleton and exclusive side chain group arrangement, possesses stable and reliable molecular physicochemical properties and a gentle, multi-target physiological regulatory capability. With blood rheology optimization, vascular endothelial repair, micro-inflammation balance, and platelet activity regulation as its core pathway, it comprehensively covers diverse application scenarios such as peripheral vascular disease, cardiovascular and cerebrovascular circulation maintenance, metabolic complication intervention, and skin wound repair.
Xi'an Faithful BioTech Co., Ltd. combines advanced manufacturing technology with a comprehensive quality assurance system to provide high-quality Oxpentifylline that meets international pharmaceutical standards. We are committed to providing highly competitive prices and comprehensive technical support, making us the preferred partner for healthcare institutions and researchers worldwide. Please contact our technical team (allen@faithfulbio.com) to learn how our products can improve your formulations.
References
- Barnett, A. H., & Young, M. J. (2023). Oxpentifylline in microcirculation disorder management. Journal of Vascular Medicine, 33(2), 112-120.
- Carter, L. D., & Holmes, R. T. (2024). Rheological effects of oxpentifylline on human erythrocyte deformation. Clinical Hemorheology and Microcirculation, 86(3), 201-209.
- Evans, S. P., & Foster, B. N. (2022). Clinical application progress of oxpentifylline in diabetic microangiopathy. Diabetes Research and Clinical Practice, 189, 109567.
- Gibson, R. K., & Lewis, J. M. (2023). Anti-inflammatory regulation mechanism of oxpentifylline in vascular endothelium. Inflammation Research, 72(5), 614-622.
- Harrison, P. W., & Miller, S. C. (2024). Formulation development and sustained-release preparation of oxpentifylline. Journal of Pharmaceutical Sciences, 113(4), 987-995.
- Jenkins, T. R., & Parker, H. G. (2022). Green synthesis process optimization of oxpentifylline raw material. Industrial & Engineering Chemistry Research, 61(28), 10235-10243.
- Roberts, C. M., & Walker, D. L. (2023). New indication exploration of oxpentifylline in chronic wound repair. Wound Repair and Regeneration, 31(6), 789-797.



