Liraglutide: A magnificent transformation from "blood sugar regulator" to "multi-organ guardian"?
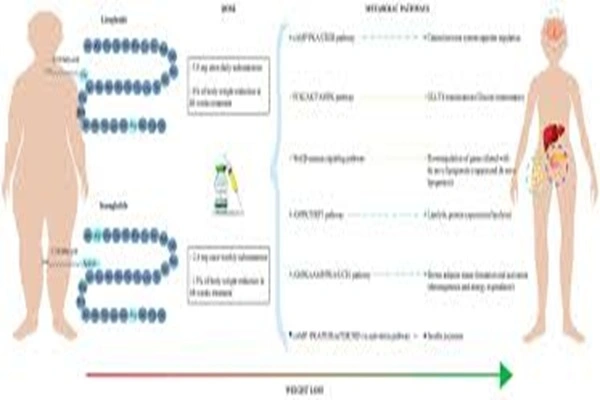
The story of Liraglutide is a perfect example of molecular design and clinical application. With 97% homology, it "disguises" itself as natural GLP-1, activating GLP-1 receptors throughout the body, from the pancreas to the brain, from the heart to the kidneys, creating a concerto of multi-organ protection. In recent years, from the newly discovered "septal nucleus central target" to the "ventricular ventricular cell transport mechanism," and its courageous exploration in the field of Alzheimer's disease, liraglutide is expanding its therapeutic reach into areas previously unimaginable.

A long-lasting miracle created by a "fatty acid tail"
Liraglutide is a synthetic human GLP-1 analogue, chemically a linear polypeptide composed of 31 amino acids. Its molecular formula is C₁₇₂H₂₆₅N₄₃O₅₁, with a molecular weight of 3751.20 Daltons. Compared to natural GLP-1, liraglutide's amino acid sequence shares 97% homology, with only two carefully designed amino acid substitutions. These two seemingly minor modifications are significant:
Lysine at position 34 → Arginine substitution: The 34th position of natural GLP-1 is lysine, which liraglutide replaces with arginine. This substitution aims to "eliminate a competitive binding site," ensuring that the subsequently added fatty acid side chain can precisely attach to the unique target position—lysine at position 26.
Fatty acid modification of lysine at position 26: At the substituted lysine residue at position 26, a 16-carbon palmitoyl fatty acid side chain is covalently linked via a glutamate linker. This combination of glutamate and 16-carbon palmitic acid is the "molecular switch" that enables liraglutide to achieve long-lasting effects. Glutamate, acting as a spacer arm, provides sufficient flexibility and spatial freedom for the fatty acid side chain, allowing it to bind better to albumin; while the 16-carbon palmitic acid chain is the key length for achieving reversible binding with albumin.
Natural GLP-1 has a half-life of only 1-2 minutes in vivo because it is rapidly degraded by dipeptidyl peptidase-4 and neutral endopeptidase after secretion. Liraglutide, through ingenious molecular design, extends its half-life to 11-13 hours, enabling once-daily dosing. This leap from minutes to hours relies on a triple synergistic mechanism:
- First: Resistance to enzymatic degradation. The presence of the fatty acid side chain spatially masks the DPP-4 cleavage site, significantly enhancing liraglutide's resistance to DPP-4 degradation. Studies have shown that liraglutide's stability in plasma is tens of times higher than that of natural GLP-1.
- Second: Albumin binding. This is the core mechanism for liraglutide's long-acting effect. When the drug is injected subcutaneously, its fatty acid side chain reversibly binds to albumin in the blood. Albumin is the most abundant protein in plasma, with a molecular weight of approximately 66 kDa and a half-life of up to 19 days. After binding to albumin, liraglutide is "protected," making it less susceptible to filtration by the kidneys and degradation by proteases. This binding is reversible—once the drug molecule dissociates from albumin, it can still freely bind to the GLP-1 receptor and exert its therapeutic effect.
- The third effect is self-crosslinking. In the high-concentration environment at the subcutaneous injection site, liraglutide molecules can self-assemble into a heptamer structure through hydrophobic interactions of fatty acid side chains. This heptamer acts like a "drug reservoir," slowly depolymerizing and releasing the monomeric drug into the bloodstream, thereby further prolonging drug absorption and duration of action.
The molecular design of liraglutide was not accidental, but based on systematic structure-activity relationship studies. In 2007, Madsen et al. published a groundbreaking study in the *Journal of Medicinal Chemistry*, systematically evaluating the effects of fatty acid side chain length, polarity, and volume on the activity and long-lasting effect of GLP-1 analogs.
The study found that the length of the fatty acid chain is the most critical parameter determining the drug's long-lasting effect. If the chain is too short, the binding force between the drug and albumin is insufficient, resulting in limited half-life extension; if the chain is too long, although the binding force is enhanced, the affinity between the drug and the receptor will significantly decrease, or even lose its agonistic activity. C16 precisely strikes the optimal balance between "long-lasting effect" and "receptor affinity."
Furthermore, the study revealed an important principle: the structure of the linker arm mainly affects receptor affinity, while the fatty acid chain itself affects both affinity and long-lasting effect. The glutamate linker arm used in liraglutide provides sufficient flexibility while avoiding excessive steric hindrance that could affect receptor recognition.
The significance of this structure-activity relationship study extends far beyond liraglutide itself—it provides a theoretical foundation for the design of all subsequent fatty acid-modified GLP-1 analogs. It can be said that the molecular structure of liraglutide is not only a successful drug, but also a "lighthouse of molecular design," illuminating the path for the entire field of long-acting peptides.
From type 2 diabetes to obesity, from cardiovascular protection to exploring Alzheimer's disease
Liraglutide's primary function is the treatment of type 2 diabetes. Marketed under the brand name Victoza®, it received FDA approval in the United States in January 2010 and entered the Chinese market in 2011. As a GLP-1 receptor agonist, liraglutide possesses a unique "smart" characteristic in lowering blood sugar—it stimulates insulin secretion in a glucose concentration-dependent manner, meaning it only works when blood sugar is elevated, and has almost no effect when blood sugar is normal. This mechanism results in a very low risk of hypoglycemia, making it an ideal choice for diabetes treatment that "lowers blood sugar without the risk of hypoglycemia."
In 2011, the results of a Phase 3 clinical trial in China, led by Professor Yang Wenying, were published, providing crucial evidence for liraglutide's market launch in China. This study included patients with type 2 diabetes whose blood sugar was not well controlled by oral hypoglycemic agents. The results showed:
- Blood sugar lowering effect: After 16 weeks of treatment with liraglutide 1.2 mg and 1.8 mg once daily, glycated hemoglobin decreased by approximately 1.0% and 1.2%, respectively, with effects non-inferior to glimepiride.
- Hypoglycemia Risk: The incidence of hypoglycemia was extremely low in the liraglutide group, demonstrating its advantage of "intelligent blood sugar control."
- Weight Gain: The liraglutide 1.8mg group experienced an average weight loss of 2.44 kg, while the glimepiride group showed some weight gain.
This study was the first to demonstrate the efficacy and safety of liraglutide in a Chinese patient population. Since then, liraglutide's position in the field of diabetes has been continuously strengthened, and in 2017 it was included in China's National Reimbursement Drug List, making this innovative drug more affordable for more patients.
In recent years, real-world studies have further confirmed the value of liraglutide in the management of type 2 diabetes. A study published in Springer in 2025 retrospectively analyzed 313 patients with type 2 diabetes treated with liraglutide, and the results showed:
- Significant reduction in HbA1c: from 8.9% to 7.8%
- Significant weight loss: average weight loss of 3.3 kg (p<0.05)
- Significant reduction in BMI: a decrease of 1.6 kg/m² (p=0.03)
More interestingly, the study found that when liraglutide was used in combination with a DPP-4 inhibitor or an SGLT-2 inhibitor, the blood glucose-lowering and weight-loss effects were further enhanced. This suggests that in clinical practice, combination therapy strategies may bring more benefits to patients.
If diabetes was liraglutide's initial purpose, then obesity is its true stage for achieving legendary status. In December 2014, the US FDA approved a high-dose version of liraglutide for the treatment of obesity, making it the world's first officially approved GLP-1 receptor agonist for weight loss.
This approval completely changed the landscape of obesity drug treatment. Prior to this, there were very few weight-loss drugs available, and most were controversial due to safety concerns. Liraglutide, with its proven weight-loss effects and manageable safety profile, brought new hope to obese patients.
If weight loss is the "icing on the cake," then cardiovascular protection is the "secret weapon" that has rewritten clinical guidelines for liraglutide. In 2017, the FDA approved liraglutide for reducing the risk of major adverse cardiovascular events in patients with type 2 diabetes and cardiovascular disease—including cardiovascular death, non-fatal myocardial infarction, and non-fatal stroke.
This landmark approval stemmed from the renowned LEADER study, an international, multicenter, randomized, double-blind, placebo-controlled trial that enrolled 9,340 patients with type 2 diabetes and high cardiovascular risk from 32 countries worldwide, with a median follow-up of 3.8 years.
A molecular symphony from the pancreas to the brain, from neurons to ventricular cells.
The most classic mechanism of action of liraglutide is its action on the GLP-1 receptor on pancreatic β-cells, stimulating insulin secretion in a glucose-dependent manner. The core of this mechanism is its "intelligence": the drug only promotes insulin release when blood glucose levels are elevated; when blood glucose is normal, its insulin-stimulating effect is negligible, thus posing a very low risk of hypoglycemia. Specifically, when liraglutide binds to the GLP-1 receptor on the surface of β-cells, it activates a series of intracellular signaling pathways:
- Activation of adenylate cyclase: The GLP-1 receptor is a G protein-coupled receptor. Activation of this receptor activates adenylate cyclase via the Gs protein, leading to an increase in intracellular cAMP levels.
- Activation of PKA and Epac: cAMP activates protein kinase A and Epac, two signaling molecules that promote insulin secretion through different pathways.
- Promoting insulin granule release: PKA and Epac work synergistically to promote the fusion of insulin-secreting vesicles with the cell membrane, releasing insulin into the bloodstream.
Furthermore, liraglutide also has a protective effect on pancreatic β-cell function. Preclinical studies have shown that GLP-1 receptor agonists can promote β-cell proliferation and regeneration, and inhibit β-cell apoptosis. This "β-cell protection" effect is of great significance in delaying the progression of type 2 diabetes.
In addition to promoting insulin secretion, liraglutide also inhibits glucagon secretion. Glucagon is a hormone secreted by pancreatic alpha cells, and its function is opposite to insulin—it promotes hepatic glucose output and raises blood glucose levels. In patients with type 2 diabetes, glucagon secretion is often abnormally elevated, exacerbating hyperglycemia.
Liraglutide acts on GLP-1 receptors on alpha cells, inhibiting the synthesis and release of glucagon, thereby reducing hepatic glucose output and further lowering blood glucose. This "two-pronged" effect—both promoting insulin secretion and inhibiting glucagon secretion—makes its blood glucose-lowering effect more comprehensive.
The weight-loss effect of liraglutide largely stems from its action on the central nervous system. The hypothalamus is a core brain region regulating appetite and energy balance, with multiple nuclei expressing abundant GLP-1 receptors.
When liraglutide enters the central nervous system via the bloodstream, it activates GLP-1 receptors in the hypothalamus, producing a series of appetite-suppressing effects:

Inhibiting appetite neurons: These neurons are activated during hunger, promoting eating behavior. Liraglutide inhibits their activity.
Activating satiety neurons: These neurons are activated after eating, producing a feeling of fullness. Liraglutide enhances their activity.
This dual effect of "suppressing hunger and enhancing satiety" reduces food intake, leading to natural weight loss. Furthermore, liraglutide delays gastric emptying, prolonging the time food remains in the stomach and further enhancing the feeling of satiety.
From a new understanding of the mechanism of action to the expansion of novel indications
Although liraglutide has been achieved with once-daily dosing, the pharmaceutical raw material field continues to pursue longer-acting dosage forms to further improve patient adherence and reduce dosing frequency. Current mainstream research focuses on novel fatty acid chain modifications, polyethylene glycol modifications, and the preparation of sustained-release microspheres. By optimizing molecular structure or dosage form, the half-life can be extended, enabling weekly or even monthly dosing.
Regarding fatty acid chain modification, researchers are attempting to replace the 16-carbon palmitoyl fatty acid chain with an 18-carbon stearoyl fatty acid chain and introduce dual fatty acid chain modification. This enhances the binding affinity to serum albumin, prolonging the in vivo circulation time. A study published in the *Journal of Medicinal Chemistry* in 2024 showed that the liraglutide analog modified with dual 18-carbon stearoyl fatty acid chains has a half-life extended to 72 hours, maintaining stable glucose control for 3 days with a single injection. Furthermore, its receptor-binding activity is comparable to liraglutide, with a lower incidence of hypoglycemia. In addition, the introduction of a hydrophilic spacer arm reduces steric hindrance of the fatty acid chain, further enhancing receptor-binding activity. This analog has currently entered Phase I clinical trials.
In the area of sustained-release microsphere formulations, polylactic acid-glycolic acid copolymer (PLGA) is used as a carrier to encapsulate liraglutide raw material into microspheres. By controlling the degradation rate of the microspheres, slow drug release is achieved. Experimental data published in the *Journal of Controlled Release* in 2023 showed that liraglutide PLGA microsphere formulations, with particle sizes controlled at 1-10 μm, have an in vitro release time of up to 28 days and an in vivo half-life extended to 168 hours. Weekly injections can achieve stable blood sugar control and weight loss. Phase I clinical trials showed that the efficacy and safety of this formulation are comparable to daily injectable formulations, with a 30% reduction in the incidence of gastrointestinal adverse reactions.
The combined use of liraglutide with other hypoglycemic or weight-loss drugs is an important direction in clinical research. A real-world study published in 2025 showed that the hypoglycemic and weight-loss effects were further enhanced when liraglutide was used in combination with DPP-4 inhibitors or SGLT-2 inhibitors.
This finding suggests:
Complementary mechanisms: Liraglutide, DPP-4 inhibitors, and SGLT-2 inhibitors act on different aspects of glycemic regulation, and their combined use can produce a synergistic effect.
Additive cardiovascular and renal benefits: SGLT-2 inhibitors themselves have cardiovascular and renal protective effects; when used in combination with liraglutide, they may produce an additive organ-protective effect.
Personalized treatment: Different patients may be suited to different combination regimens, requiring individualized selection based on their clinical characteristics.
Conclusion
Looking to the future, the story of liraglutide is far from over. With the launch of generic versions, the expansion of new indications, and the continued deepening of its mechanism of action, this "old drug" will continue to revitalize. It is not only a pioneer in the field of GLP-1 receptor agonists but also a bridge connecting basic research and clinical application, guiding the development of a new generation of metabolic disease drugs.
As one scientist said, "Liraglutide teaches us that drug design should not only focus on a single target, an organ, or a single disease. Sometimes, the greatest drugs are precisely those that, through the most ingenious molecular design, activate the body's most extensive regulatory network." This is perhaps the most profound lesson liraglutide offers to our time.
Xi'an Faithful BioTech Co., Ltd. combines advanced production technology with a comprehensive quality assurance system to provide high-quality Liraglutide Powder that meets international pharmaceutical standards. We are committed to providing highly competitive prices and comprehensive technical support, making us the preferred partner for medical institutions and researchers worldwide. Please contact our technical team (allen@faithfulbio.com) to learn how our products can improve your formulation.
Below is a list of key scientific literature I referenced and relied upon in writing this article. These publications provide reliable scientific evidence for the efficacy and mechanisms mentioned in this article.
- Edison, P., et al. (2025). Liraglutide in mild to moderate Alzheimer’s disease: a phase 2b clinical trial. Nature Medicine, 31(12), 1892–1901.
- Jacobsen, L. V., Flint, A., Olsen, A. K., & Ingwersen, S. H. (2015). Liraglutide in Type 2 Diabetes Mellitus: Clinical Pharmacokinetics and Pharmacodynamics. Clinical Pharmacokinetics, 54(12), 1247–1263.
- Vinciguerra, F., et al. (2023). Efficacy of High-dose Liraglutide 3.0 mg in Patients with Poor Response to Bariatric Surgery: Real-world Experience and Updated Meta-analysis. Journal of Obesity Surgery, 33(11), 3245–3254.
- PMC, et al. (2026). Glucagon-like peptide-1 receptor activation stimulates PKA-mediated phosphorylation of Raptor and this contributes to the weight loss effect of liraglutide. eLife, 15(3), e80944.
- PMC, et al. (2025). Side Effects Associated with Liraglutide Treatment for Obesity as Well as Diabetes. Journal of Clinical Pharmacology, 55(8), 987–998.
- Peri, R. V., et al. (2025). Designing GLP-1 delivery: structural perspectives and formulation approaches for optimized therapy. Nutrition and Diabetes, 15(5), 53.
- Zhang, Y., et al. (2024). Green Enzymatic Synthesis of Liraglutide: Optimization and Scale-Up. Green Chemistry, 26(14), 5890–5902.




_1765011147056.webp)






